The menopause is the end of the female reproductive life. It is a physiological process which begins as perimenopause at around the age of 45 and progresses until the final menses and the end of fertility (UK average age is 51).
The menopause comes with a range of classical symptoms experienced by most women, which can become troublesome in daily life and result in the woman seeking medical assistance.
In this article we shall cover the physiology of the menopause, the classical clinical features and hormone replacement therapy.
Changes During the Menopause
Hormonal Changes
The menopause is characterised by a reduction of circulating oestrogen. This is the result of reduced sensitivity of the ovary to circulating gonadotropins (FSH and LH) as a result of a marked decrease in available binding sites due to the reduction in follicle numbers.
The result of this reduced sensitivity is the reduction in oestrogen secretion and an increase in anovulatory cycles.
Levels of FSH and LH increase significantly during the menopause due to low levels of circulating oestrogen, thus removing negative feedback on the hypothalamus and the pituitary gland. The decrease in developing follicles also reduces the amount of inhibin released – causing an enhanced rise of FSH.
Women progressing toward the menopause (perimenopausal) often experience a variety of symptoms such as hot flushes, urinary incontinence and increased UTIs as well as irregular vaginal bleeding. Some of this bleeding is the result of menstruation from ovulatory cycles. Other bleeds are from anovulatory cycles where endometrium has proliferated under oestrogen without the balance of progesterone from the corpus luteum after ovulation.
Progesterone is required to support the endometrium so when ovulation does not occur the endometrial lining breaks down. This is termed oestrogen breakthrough bleeding and can happen as frequently as every fortnight in perimenopausal women.
As levels of oestrogen decrease both of these types of bleeding gradually cease.
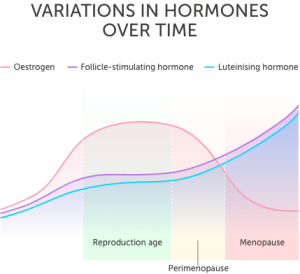
Fig 1 – Variations In Hormone Levels from Reproduction to Menopause
Vasomotor Changes
75% of women going through menopause experience hot flushes. These occur with a red flush starting on the face and spreading down the neck and chest.
These are associated with peripheral vasodilation and a transient rise in body temperature. The exact mechanism is unknown, but it is thought to be due to pulsatile LH release influencing central temperature control.
Urogenital Changes
The uterus and vagina are both tissues which are maintained by circulating oestrogen. After the menopause there is marked atrophy of the vagina and thinning of the myometrium. There is also thinning of vaginal walls and dryness, this can result in dyspareunia (pain during sex).
The bladder and urethra share embryological derivation with the uterus and vagina and so these tissues also atrophy with the decrease in circulating oestrogen. This leads to symptoms of urinary incontinence and an increase in urinary tract infections.
Bone Density
Oestrogen protects bone mass and density through reducing the activity of oesteoclasts. With the drop in oestrogen this balance is tipped and there is an increase in bone reabsorption. This results in an acceleration of age-related loss of bone density and an increased frequency in fractures, especially of the wrist and hip.
Ischaemic Heart Disease
Oestrogen offers a protective effect against heart disease. It is thought that oestrogen reduces levels of LDL cholesterol whilst raising HDL cholesterol. After the menopause women experience the same frequency of cardiovascular disease as men.
Defining the Menopause
The menopause is defined when a woman has had amenorrhoea (no menstruation) for 12 months. Before this time there is still the possibility of fertility and the appropriate precautions should still be taken regarding contraception. If menopause occurs in a woman aged between 40-45 this is termed ‘Early Menopause’.
Apart from the loss of fertility there are no immediate health risks, although there is an increased risk of osteoporosis, dementia and cardiovascular disease if HRT is not appropriately managed.
Clinical Relevance – The Menopause
The menopause is often diagnosed using blood tests to measure hormone levels. Typically FSH is measured, and a level of above 40 Iµ/L is indicative of the menopause. Measuring oestrogen is generally not helpful as levels may continue to fluctuate even after the menopause.
Some women choose to allow the menopause to progress naturally and find the symptoms tolerable. But for those who cannot tolerate the symptoms, Hormone Replacement Therapy (HRT) is often offered. It is available in various formulations, including daily tablets, transdermal patches or an oestrogenic vaginal ring. This allows women to use the formulation that best suits them and their symptoms.
However, it is important to remember that HRT carries with it a modest increase in the risk of breast, endometrial and ovarian cancers. There is also an increased risk of venous thromboembolism whilst on HRT due to the pro-thrombotic effect of oestrogen. Alongside this is an increased risk of ischaemic stroke, especially in women aged over 60 years.
Clinical Relevance – Premature Ovarian Insufficiency
Unlike the menopause, premature ovarian insufficiency can be a reversible condition so is not termed an early menopause. It occurs in women under the age of 40 and is characterised by low oestrogen, high gonadotropins and amenorrhoea.
The exact cause varies, although in some women FSH receptor mutations have been identified or follicular dysfunction occurs.
Treatment often involves a multidisciplinary team to manage the psychological impact of the condition alongside the physical symptoms. HRT is the main treatment, alongside monitoring for cardiovascular disease and osteoporosis.
