Urinary incontinence is the involuntary leakage of urine. It is a common and distressing problem, which can have a large impact on quality of life
There are several triggers, types and causes – with most cases occurring in elderly, postmenopausal, parous women.
In this article, we shall look at the classification, clinical features and management of urinary incontinence.
Classification and Pathophysiology
There are two main types of urinary incontinence; stress incontinence and urge incontinence – with mixed incontinence describing patients with features of both types (most common).
Stress Incontinence
Stress incontinence is defined as the involuntary leakage of urine during increased intra-abdominal pressure (in the absence of a detrusor contraction).
It is typically seen after childbirth, which is the most common causative factor, having resulted in denervation of the pelvic floor. Other risk factors include oestrogen deficient states, pelvic surgery and irradiation.
Urge Incontinence
Urge incontinence (also known as overactive bladder syndrome) is the presence of urgency, usually with frequency and nocturia, in the absence of urinary tract infection or any other obvious pathology.
Urodynamic testing typically shows over-activity of the detrusor muscle. This is the type of incontinence seen in neurological conditions like multiple sclerosis or spina bifida – however most cases are idiopathic and some caused by pelvic/incontinence surgery itself.
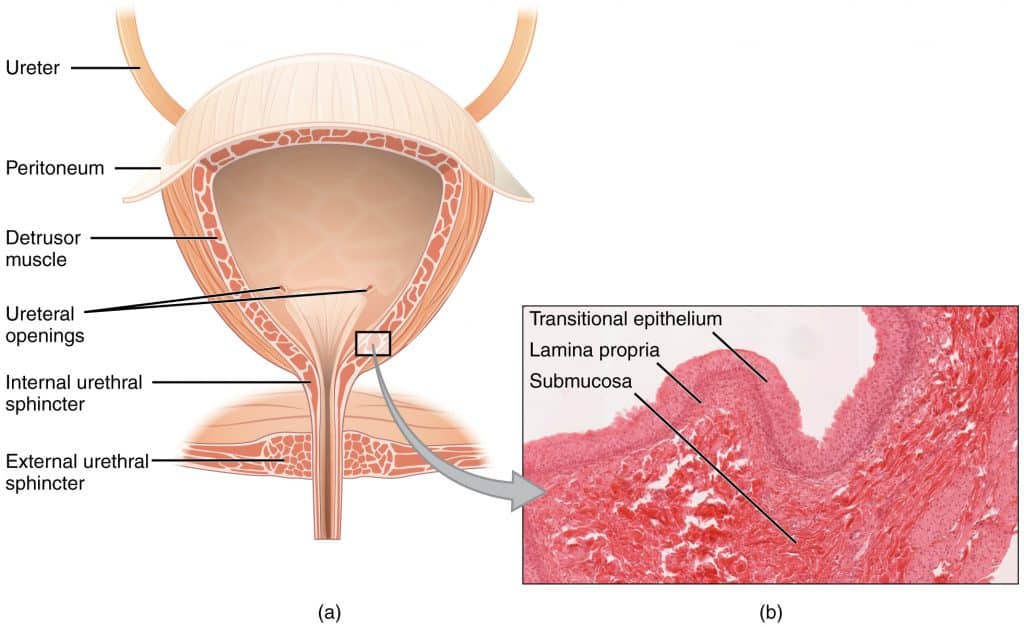
Fig 1 – Anatomy of the bladder. Over-activity of the detrusor muscle is implicated in urge incontinence.
Other Causes
There are other causes that should be considered in the assessment of any patient with urinary incontinence:
- Overflow incontinence – leakage of urine from an overfull urinary bladder, often in the absence of any urge to urinate.
- Bladder fistulae – opening between the bladder and another organ (e.g. the vagina or rectum).
- Urethral diverticulum – out-pocketing of the urethra into the anterior vaginal wall.
- Congenital anomalies – e.g. ectopic ureter.
- Functional incontinence – physical or mental barriers that prevent the patient reaching the toilet (e.g immobility, dementia).
- Temporary incontinence – due to reversible factors such as constipation and urinary tract infection.
Clinical Features
Stress Incontinence
Stress urinary incontinence is the involuntary leakage of urine on exertion.
Typically, this occurs when intra-abdominal pressures rise and this is communicated through to the bladder, resulting in leakage on coughing, sneezing or exercise. As such, this is the symptom with which women present. The leakage is often a small volume coinciding with physical stress
On examination, prolapse of the urethra and anterior vaginal wall may be present. Also, asking the woman to cough with a semi-full bladder may demonstrate the incontinence.
Urge Incontinence
Urge incontinence describes the sensation of urgently needing to pass urine, resulting in involuntary leakage.
Patients will often complain of urgency (“If they have to go they have to go’’), frequency and nocturia. There are often trigger factors such as hearing running water, cold weather, etc. There are typically large volumes of leakage compared to stress incontinence.
Bladder contractions may be triggered by coughing or sneezing which can lead to the false assumption that stress incontinence is present.
| Symptom | Description |
| Day time frequency | A perception of voiding urine too often during the day |
| Nocturia | Having to wake one or more times during the night to pass urine |
| Urgency | A sudden and compelling desire to pass urine, which is difficult to defer |
Investigations
In a patient presenting with urinary incontinence, the primary investigation must to be exclude infection of the urinary tract. As is well known, this is the classic mimic for incontinence and there is considerable overlap of symptoms.
The Investigation of both urge and stress incontinence is through frequency charts and urodynamic studies:
- Frequency/volume charts
- Stress – normal frequency and bladder capacity
- Urge – increased frequency
- Urodynamic studies – performed in stress urinary incontinence when considering surgery to confirm the diagnosis and rule out concomitant detrusor over-activity.
Management
The management for urinary incontinence can be divided in conservative, medical and surgical therapies.
Stress Urinary Incontinence
Conservative
- Lifestyle changes – weight loss, caffeine reduction and smoking cessation.
- Treatments of risk factors – such as conditions that raise the intraabdominal pressure (e.g chronic cough).
- Supervised pelvic floor muscle training – undertaken for a period of at least three months. Pelvic floor muscle training can be continued after three months if it has been beneficial to the patient.
Surgical
- Burch colposuspension – this is now rarely performed due to the introduction of vaginal tapes. It involves inserting sutures between the paravaginal fascia and Cooper’s ligament.
- Laparoscopic colposuspension – similar to the above procedure but performed laparoscopically as opposed to open.
- Tension free vaginal tape (TVT) – the most commonly performed operation with a high objective cure rate. It involves a tape being placed under the mid urethra via a small vaginal incision.
- There has been recent controversy over this procedure with many women reporting complications of erosions into the vagina, urethra and bladder resulting in chronic pelvic pain.
Medical
- Duloxetine – licensed for the treatment of moderate to severe incontinence. This can be used for women who do not wish to have surgery or are not suitable for surgery
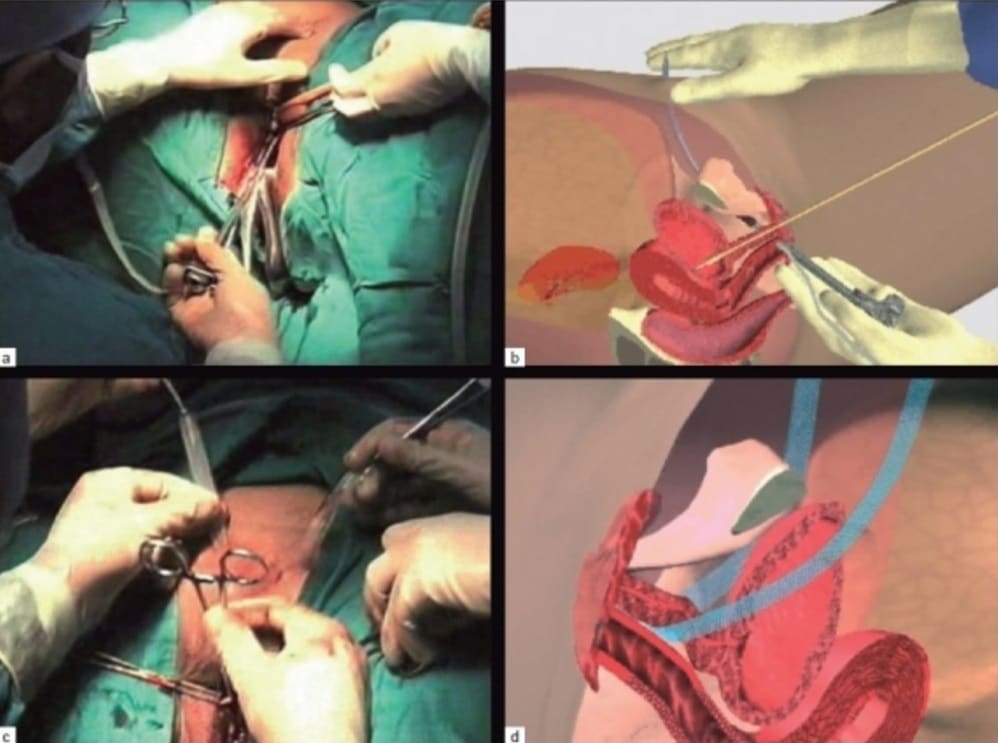
Fig 2 – Stages of a tension-free vaginal tape. (a) TVT needle insertion on left side, with catheter and metal guide on same side, (b) Schematic insertion of TVT tape, (c) Adjusting tension free TVT, (d) Mechanism of action of mid-urethral application TVT.
Urge Incontinence
Conservative
- Lifestyle changes – advice on fluid intake and aversion to caffeine and diuretics (including alcohol)
- Bladder retraining
Medical
- Anticholinergic medication – oxybutynin, solifenacin, tolterodine.
- Be mindful of the side effects (xerophthalmia, xerostomia, constipation, blurred vision, arrhythmias, confusion) and the contraindications (acute angle closure glaucoma, myasthenia gravis, GI obstruction, etc.)
- Intravaginal oestrogens – may ameliorate symptoms for those with vaginal atrophy.
- Botulinum toxin A
- Neuromodulation & sacral nerve stimulation
Surgical
- Detrusor myomectomy and augmentation cystoplasty.
- This is reserved only for those with debilitating symptoms.
Summary
- Urinary incontinence can be subdivided into stress incontinence, mixed and urge incontinence.
- It is important to remember that these are debilitating conditions for patients and a major disruption to their lives
- Exclusion of urinary tract infection must be done in any patient presenting with incontinence.
- Conservative management is indicated in almost all cases
- Medical therapy is indicated in both types of incontinence but surgical intervention is only to be considered as a last resort in those patients with urge incontinence.
